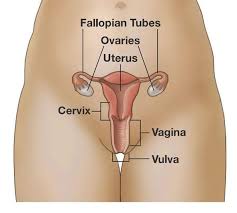
Cervix is a part of female reproductive tract. It is the lower narrow part of uterus or "the womb" which connects to the vagina.
Do not confuse Cervix as a part of neck
The commonest cancer among women in India and the second most common worldwide. Almost 1,35,000 new women are diagnosed with cancer cervix every year in India alone.
Every 7 mins one women dies of cervical cancer of which every fourth is an Indian.
Do not ignore these symptoms, they can lead to early diagnosis
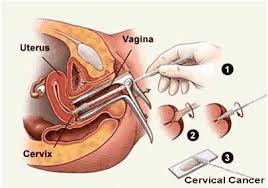
Cervical screening is a way of detecting early changes to cells of the cervix. It's not a test for cancer, but it can help prevent cervical cancer from developing by identifying early abnormalities that could become cancer if left untreated. The first step in cervical screening is to take a sample of cells from the cervix using a simple test known as Pap smear.
Cervical screening doesn't diagnose cancer. It's used to detect early changes in cells of the cervix, which may develop into cancer in the future.
It is taken during an internal examination of the vagina. It is not painful and takes only a few minutes. An instrument called the speculum is inserted to hold the walls of the vagina and some cells are gently taken, using a spatula, and smeared on a glass slide. This slide is tested in a laboratory for abnormal cells. The results may take a few days. Schedule your Pap when you are not having a menstrual period. It is best to abstain from intercourse and avoid use of tampons or douches for two days before your Pap test. If you have an abnormal result, it is extremely important to follow-up for the recommended testing. Even after a normal Pap test, it is still important to report any symptoms of abnormal vaginal bleeding, discharge or pain to your doctor and call to be seen right away.
Best time to have the test is midway between periods.
All women between the ages of 21 and 70 years who have ever been sexually active. Test should be done once in three years. Pap testing can be stopped after 70 years of age if previous three tests are normal.
Take the test, Not the risk
99%of cervical cancer is caused by human papilloma virus (HPV). There are over 100 types of the virus. The types that cause genital warts are known as low-risk HPV types (most common type 6 &8). The high-risk types cause cancer (type 16,18 cause 70%of the cancers). The human papilloma virus is sexually transmitted, and the possibility of contact with it increases with the number of partners a woman or her partner has had. Through regular cervical screening, the changes caused by HPV can be picked up early and any treatment needed is simple and effective. Very rarely, these changes can go on to develop into CIN or cervical cancer if they are left untreated
50% of females will be infected with HPV within 3 years of marriage.80%oftimes it gets cleared on its own
Colposcopy is an OPD procedure in which detailed examination of cervix is done under a microscope to look for abnormal areas. This is usually required if an abnormality is detected on Pap smear. The colposcopist will use a speculum, in the same way as in the screening test, to hold your vagina open. The cervix is then painted with a liquid to make the abnormal areas show up more clearly. A light is shone onto the cervix and the doctor or nurse will look through the colposcope, which stays outside your body, to examine the surface of the cervix. A small sample (biopsy) of cells may be taken from the cervix, to be looked at under a microscope.
Colposcopy takes 15–20 minutes and so is longer than the screening test. It's not usually painful, but you may feel some pain if a biopsy is taken. The biopsy may also cause some slight bleeding for a couple of days afterwards. If the abnormal area still can't be seen clearly with a colposcope, the colposcopist may arrange for you to have a cone biopsy (see below) or a large loop excision of the transformation zone
Yes – for most women. Regular cervical screening every three to five years is the best way to detect changes to the cells of the cervix. Early detection and treatment can prevent cancer from developing in around three-quarters (75%) of cases. Because of cervical screening, cancer cervix is now uncommon in western countries.
Regular cervical screening can prevent about seven or eight out of every 10 cervical cancers
Two vaccines have been produced to prevent HPV. These are called Gardasil and Cervarix. It is hoped that these vaccines will prevent at least 7 in 10 (70%) of the most common type of cervical cancer (squamous cell). The vaccine is recommended for girls 9 to 12 years of age. It can be given upto 26 years of age. It acts best before onset of sexual activity.
Vaccines are not a substitute for screening

Yes it can be given but it may or may not benefit them. Cervarix is recommended upto 45 yrs of age. Benefits may be limited to the protection against infection of HPV genotypes with which they have not been infected.
Vaccine does not treat existing HPV infection
© 2026 Oncomed Clinic. All Rights Reserved | Developed by TbspLabs
