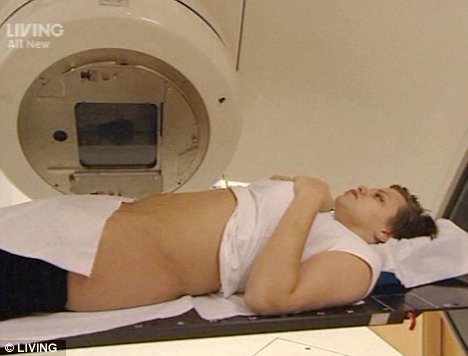
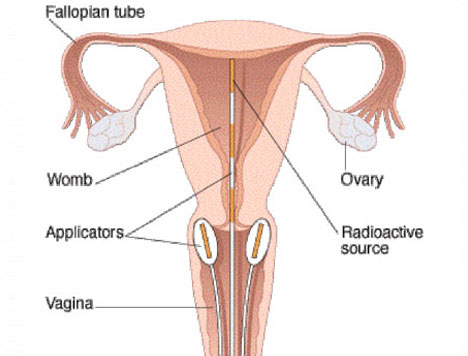
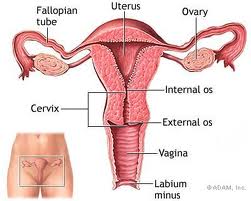
The cervix is the lower part of the womb (uterus) and is often called the neck of the womb. It joins the womb to the top of the vagina. It is possible for your doctor to see and feel the cervix during an internal (vaginal) examination.
This information is about cancer of the cervix (neck of the womb). Cancer of the womb (uterus) is different and is discussed in our section on cancer of the womb.
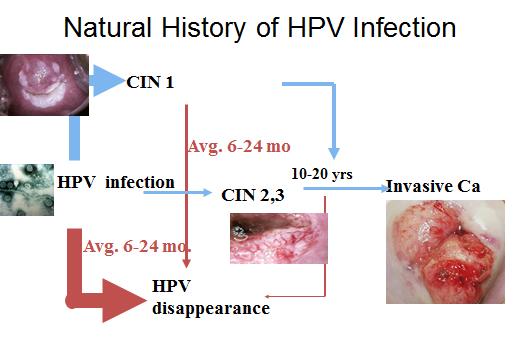
Cancer of the cervix can take many years to develop. Before it does, changes occur in the cells of the cervix. These abnormal cells are not cancerous, and are called cervical intra-epithelial neoplasia (CIN). CIN may also be referred to as dysplasia. Some doctors call these changes pre-cancerous. This means that the cells might develop into cancer in some women if they are not treated.
It is important to know that most women with CIN do not develop cancer.
The Human Papilloma Virus (HPV). HPV is a very common virus that can affect the cells of the cervix. It's mainly passed on during sex. Most women who have had sex will have the virus at some time in their life. However, in many women their immune system will get rid of the virus and they won't know they ever had it. The cervical smear can detect changes in the cells of the cervix caused by HPV infection.
There are more than 100 types of HPV and each type is identified by a number (e.g. HPV 16). Some types of the virus can cause genital warts, and other types can cause CIN in the cells of the cervix. CIN usually clears up once the immune system has got rid of the virus. In some women the virus stays for a number of years, and in a few of these women the CIN will develop into cancer if it is not treated.
The type of HPV can affect whether CIN develops or not. Only certain types, such as 16, 18, 31 and 33 (known as 'high-risk' types) seem to be associated with the development of CIN, and ultimately with cervical cancer.
Cervical cancer is the most common cancer among women from the Indian subcontinent. Even considering all the cancers among men and women together, cervical cancer ranks number one in India.
Every year almost 1, 32000 new cases are diagnosed and almost 72,000 females die of the disease
In India every 7 minutes one women is dying of cervical cancer
Usually women begin by seeing their family doctor (GP), either when they notice symptoms, or if a cervical screening test has found abnormal cervical changes. Your GP will examine you and refer you to hospital for any necessary tests and for specialist gynecological oncologist's advice and treatment.
Most women will have a test called a colposcopy. In this test doctor uses a small microscope with a light (a colposcope) to examine your cervix. If your doctor cannot see area clearly enough, you may have another test: a large loop excision of the transformation zone (LLETZ) or a cone biopsy. These are minor operations that allow doctors to remove a section of tissue from the cervix. The tissue is then sent to a laboratory to be checked under a microscope.
The tests will show whether you have cancer, and give other important information such as the stage and type of cancer. This information, as well as the physical examination and the results of further tests your doctor may recommend, will help your doctors to know which the best type of treatment for you is.
If you are diagnosed with cervical cancer, your oncologist will need to do some further tests to check your general health and see whether the cancer has spread beyond the cervix. The tests may include any of the following:
There are two main types of cervical cancer
There are other, less common type of cancer of the cervix known as adenosquamous carcinoma, clear-cell and small-cell carcinoma.
Tests will show which type of cervical cancer you have. They will give other important information such as the stage of the cancer. This information will help your doctor know which the best type of treatment for you is.
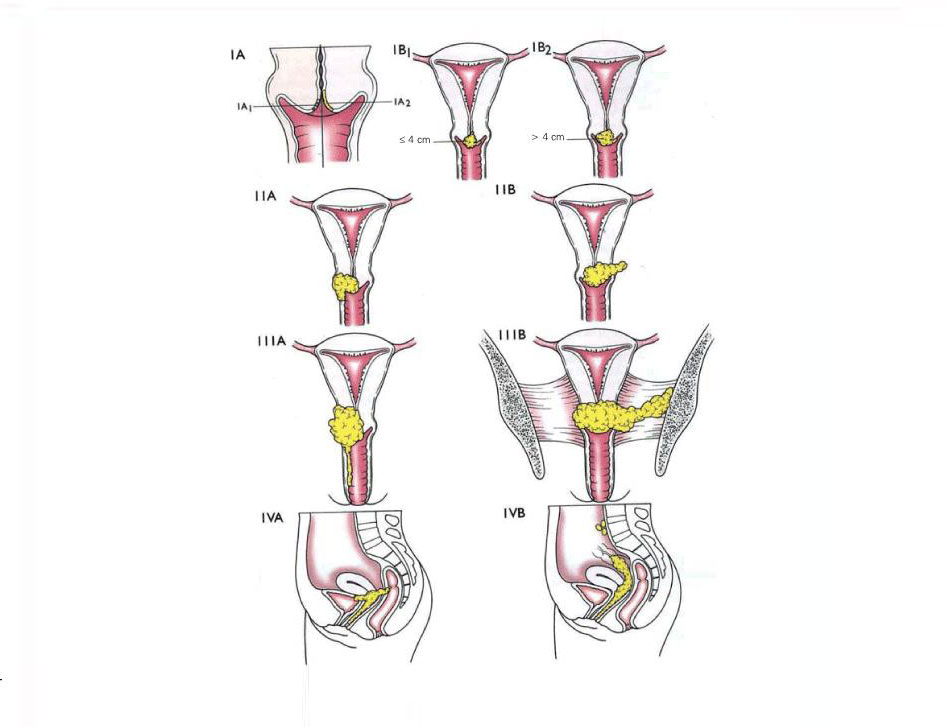
The stage of a cancer describes its size and whether it has spread beyond its original site. Knowing the extent of the cancer helps the doctors to decide on the most appropriate treatment. Cervical cancer is divided into 4 main stages.
The cancer cells are only within the cervix.
The cancer has spread into surrounding structures such as the upper part of the vagina or tissues next to the cervix
The cancer has spread to areas such as the lower part of the vagina, or tissues at the sides of the pelvic area.
The cancer has spread to the bladder or bowel or beyond the pelvic area.
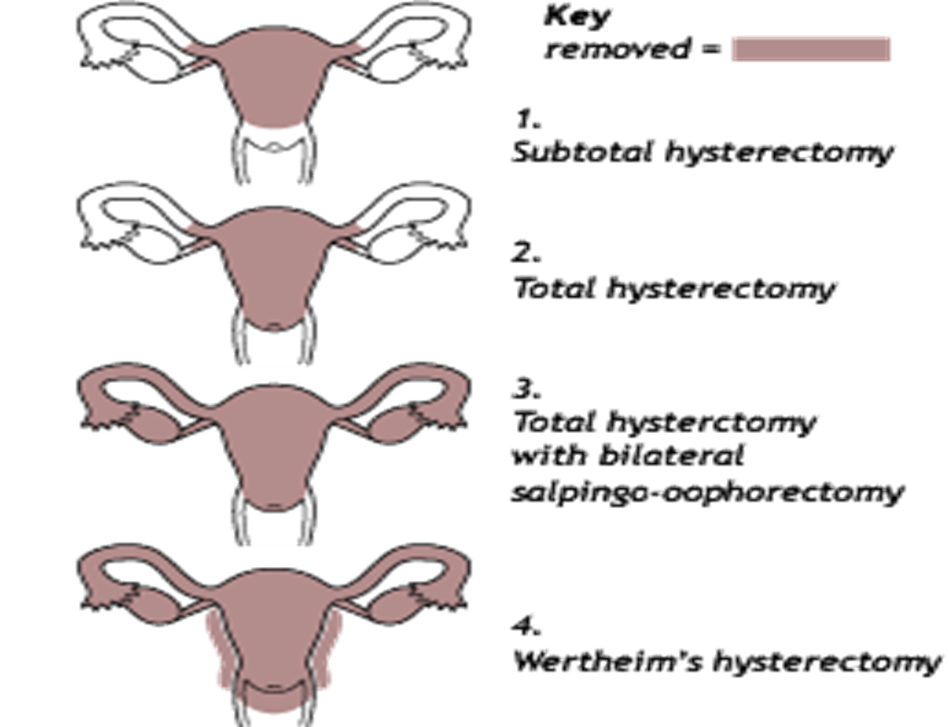
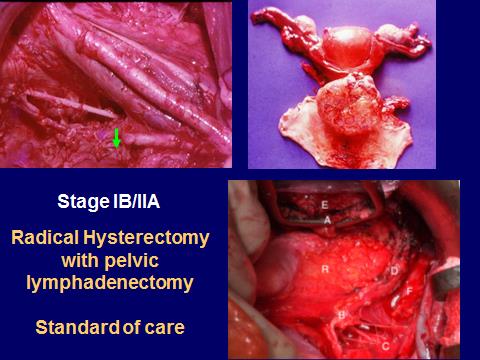
Radiotherapy may be used as an alternative to surgery for early stage cancer. It is sometimes given after surgery if there is a risk that some cancer cells may be left behind. This helps reduce the risk of the cancer coming back. Often radiotherapy is combined with chemotherapy for larger tumors in the cervix (over 4cm). This is known as chemo radiation.Chemotherapy is occasionally used before surgery, to shrink the cancer and make the operation easier, but this is not common.
If the cancer has spread beyond the cervix, and can't be cured with surgery alone, radiotherapy is usually given in combination with chemotherapy rather than surgery. Advanced and recurrent cancer Chemotherapy may be given to women whose cancer has spread to other parts of the body or if the cancer comes back after radiotherapy. It is used in this situation to try to shrink and control the cancer and relieve symptoms, to prolong a good quality of life. This is known as palliative treatment. Occasionally an operation known as a pelvic exenteration may be carried out, although this is only suitable for a small number of women. Planning treatment for cervical cancer .